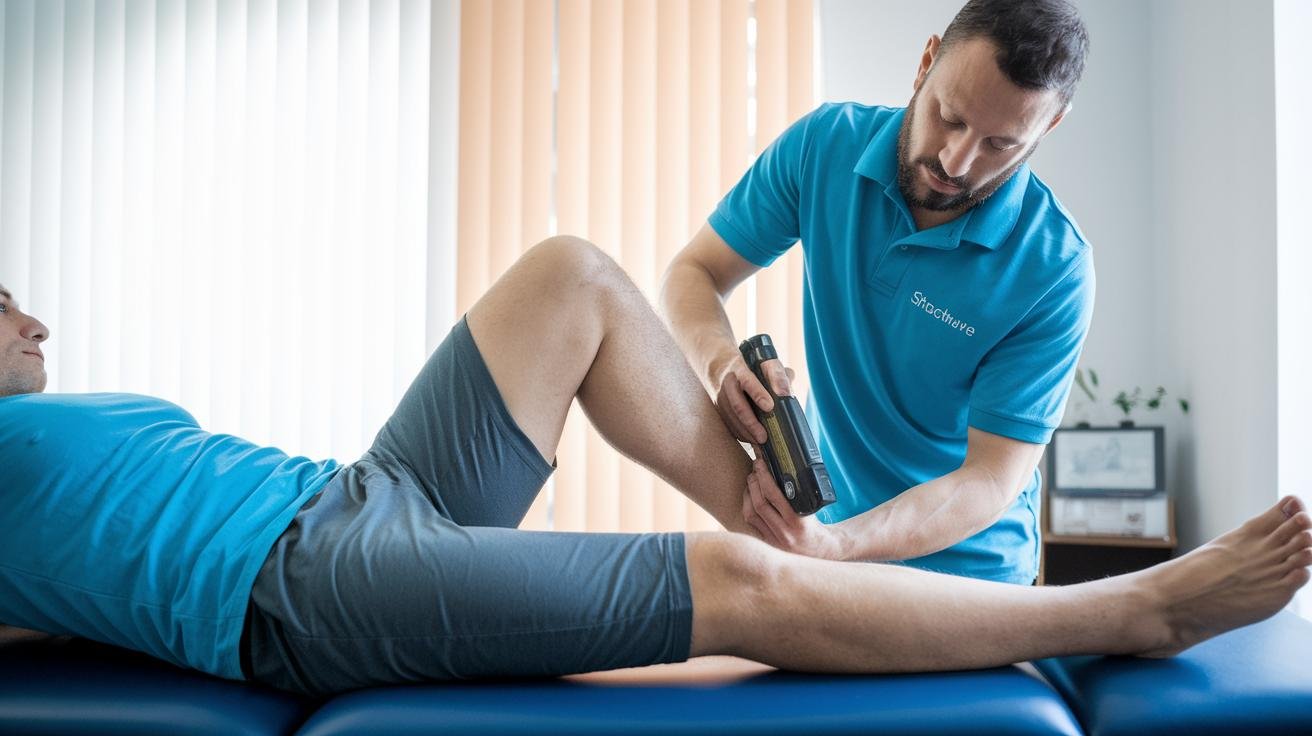
Could a quick, focused pulse replace weeks of rest and pain meds? Sometimes, yes, when it’s used the right way and matched to the injury.
Shockwave therapy (a treatment that uses short, focused pressure pulses) began by breaking up kidney stones and then moved into healing muscles, tendons, and other soft tissues. Think of it as tiny, controlled taps that wake up blood flow and nudge cells to repair, all without an incision and usually without anesthesia.
There are two main device types. Radial devices spread outward like ripples on a pond and work well for wide, surface problems. Focused devices aim deeper, like a flashlight beam, to reach tight spots under the surface.
When the device and treatment plan match the injury, shockwave therapy can speed healing, reduce pain, and shorten rehab time. That makes it a practical option for clinicians and athletes looking to get people back to daily life or sport sooner.
Shockwave Therapy Device Types & Technology Overview
Extracorporeal shockwave therapy (ESWT) is a noninvasive treatment that started out breaking up kidney stones and later moved into healing soft tissues. Think of it as short, controlled pulses of pressure that travel through the skin and nudge circulation and repair processes. No incision. Usually no anesthesia.
Manufacturers divide systems into radial shockwave therapy (RSWT) and focused shockwave therapy (FSWT). Radial units send lower-energy, outward-spreading waves measured in bar (a unit of pressure) and work across wider, more surface-level areas. Focused devices pack higher energy measured in mJ/mm² (millijoules per square millimeter) into a tight beam that reaches deeper tissue. Frequencies typically run from 1–21 Hz (pulses per second). Applicator heads commonly come in 10, 15, 20, and 35 mm sizes, and good contact with a coupling medium like ultrasound gel is key for energy to pass into the body. Wait, let me clarify that, no gel, no good transmission.
| Feature | Radial ESWT | Focused FSWT |
|---|---|---|
| Energy Delivery | Lower energy, measured in bar | Higher energy, measured in mJ/mm² |
| Penetration Depth | Superficial to mid-depth | Deeper, targeted zones |
| Typical Uses | Myofascial pain, tennis elbow, large muscle areas | Plantar fasciitis, calcific tendinopathy, delayed bone healing |
| Applicator Sizes | 10, 15, 20, 35 mm | 10, 15, 20, 35 mm (different focal heads) |
| Frequency Range | 1–21 Hz | 1–21 Hz |
Which one should you pick? Match the device to how deep and how wide the problem is. Use radial when you want broad coverage for trigger points or big muscle groups. Use focused when you need to hit deep tendon lesions, calcium deposits, or non-union fractures. Also think about cost, clinic flow, and how comfortable the patient will be, focused units often suit stubborn, deep problems while radial machines are great for general musculoskeletal rehab and quicker surface issues.
One last practical tip: good contact, the right applicator head, and an experienced operator make a big difference. Relax. Breathe. You're not alone in choosing the right tool.
Shockwave Therapy Device Clinical Effectiveness & Treatment Indications
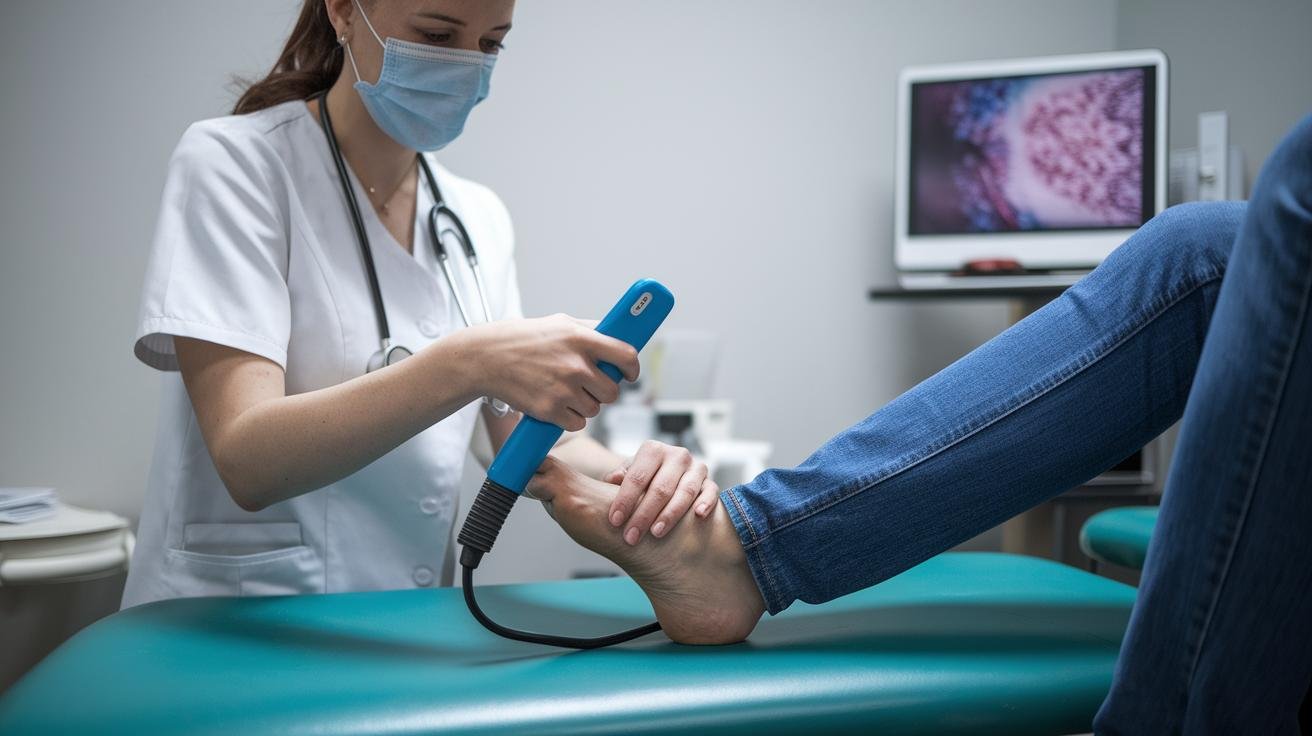
Focused shockwave therapy (FSWT) (high-energy, targeted pressure waves) has the clearest clinical backing for stubborn, slow-to-heal problems. Studies and reviews report success rates around 70 to 80 percent for conditions like plantar fasciitis, calcific shoulder tendinopathy, and non-union fractures. It’s convincing, really.
Typical FSWT care plans are short and predictable: three to four sessions, usually one week apart. Each visit delivers about 2,000 to 4,000 impulses over five to fifteen minutes. Many people feel pain ease after the first visit, with tissue remodeling and real functional gains showing up over the following weeks. Side effects are usually mild , brief pain, some redness, or a little swelling.
Radial shockwave therapy (RSWT) (lower-energy, outward-spreading pressure waves) works differently. It’s better for surface-level or wide-area issues, like large muscles and trigger-point work. Evidence supports RSWT for lateral epicondylitis (tennis elbow) and chronic myofascial pain, though overall response rates tend to be a bit lower than with focused treatments.
Clinics like radial units for busy workflows because they cover wider areas per pulse and are easy to use on big muscle groups. RSWT energy is usually reported in bar pressure, and session timing often mirrors focused protocols, so you can plan rehab the same way. Handy, simple, practical.
Common treatment indications include:
- plantar fasciitis (shockwave therapy for plantar fasciitis)
- Achilles tendinopathy (shockwave for Achilles tendinopathy)
- tennis elbow (shockwave treatment for tennis elbow)
- calcific shoulder tendinopathy
- chronic myofascial pain
How does shockwave therapy help tissue heal? The pulses boost microcirculation and metabolic activity, like a gentle, focused wake-up call to sleepy tissue. They promote neovascularization (new blood vessel growth) and stimulate collagen production to rebuild damaged structures. Treatment can also reduce muscle tone and trigger anti-inflammatory and analgesic responses, working partly through the gate control theory of pain (a way the nervous system dampens pain signals). Move more. Hurt less.
Have you ever wondered what the treatment actually feels like? Some describe a tapping or thudding that’s intense for a moment, then settles into a warm, soothing relief , like sunlight spreading across a stiff shoulder. It’s not magic, but it can be surprisingly effective.
Professional Shockwave Equipment: Features & Specifications

Start by matching the device to your clinic’s goals. Are you treating deep tendons or surface muscles? Do you need something portable for house calls, or a full-size unit that keeps a busy clinic moving? Thinking about depth of target tissue, patient comfort and patient flow will guide your choice more than brand names.
| Specification | Typical Range | Clinical Impact |
|---|---|---|
| Price | $10,000–$40,000 | Lower-cost radial units cut upfront spending; focused systems cost more but reach deeper calcifications and tendon lesions |
| Energy Output (shockwave device intensity levels) | RSWT (radial shock wave therapy): bar pressure; FSWT (focused shock wave therapy): 0.01–0.60 mJ/mm² (millijoules per square millimeter, a measure of energy density) | Higher mJ/mm² helps treat deep tendons and calcifications; bar settings are better for surface muscle work |
| Frequency (shockwave frequency range) | 1–21 Hz (pulses per second) | Higher Hz shortens treatment time; lower Hz can feel gentler and gives tissue a little recovery between pulses |
| Applicator Sizes (shockwave handpieces) | 10, 15, 20, 35 mm | Small heads focus energy on trigger points; larger heads cover broad muscles and bursae |
| Portability | Light handheld devices to trolley-mounted units | Battery-powered, cordless options help outreach care; trolley units speed patient turnover in the clinic |
User interfaces really matter for clinic speed. Look for touchscreens, preset protocols and easy parameter changes so staff can move between cases without fuss. Built-in protocols are like a recipe book: pick the condition, then tweak energy and pulse count.
Real-time feedback systems tell you pulse delivery and help keep intensity consistent. That consistency protects patients and makes your outcomes repeatable. For coupling, most clinics use clear, water-based ultrasound gel because it’s simple and familiar. Some focused systems use enclosed water coupling for steadier energy transmission.
Handpieces feel different in your hand. Test one before you buy so poor ergonomics don’t slow your workflow. Think of a handpiece like a small massage tool for tired muscles , if it’s comfy, your staff will use it more and patients will relax faster.
Oh, and one more tip: plan for throughput. If you expect a high patient volume, prioritize quick setup, preset protocols and a system that’s easy to clean between sessions. Makes the day smoother.
Shockwave Therapy Devices Improve Rehab Outcomes

Most clinical shockwave systems carry FDA (U.S. Food and Drug Administration) clearance or CE marking (Conformité Européenne). That means they meet recognized safety and performance standards. Patients usually report only mild, short-lived reactions. Think a quick, sharp snap during the pulse, a warm flush, or a little puffiness afterward.
Have you ever felt a brief sting and then relief? That’s common. Good contact with ultrasound gel and routine infection-control steps help keep treatments consistent and safe. Oh, and clear technique matters, proper coupling makes the therapy work better.
Common reasons to avoid treatment include pregnancy, bleeding disorders, or being on strong anticoagulants (blood thinners). Also skip treatment over active infections, open wounds at the site, or any known cancer near the target area. Safety first. If you’re unsure, check with the treating clinician.
Typical side effects are usually mild: transient pain, erythema (skin redness), and minor edema (mild swelling). They most often settle in a few days. If symptoms linger or worsen, contact a healthcare provider.
Device care keeps results reliable. Follow a few simple maintenance steps:
- Calibration schedule , have devices checked and calibrated every 6-12 months so energy delivery stays accurate.
- Applicator replacement , swap heads after about 1,000-3,000 pulses or whenever you see wear to avoid uneven output.
- Cleaning and disinfection , follow the manufacturer’s protocol, wipe handpieces between patients, and use single-use covers when recommended.
- Software updates , install vendor updates and protocol patches to keep presets correct and to keep traceable logs.
Train your team. Staff should get hands-on instruction and regular competency checks. Document informed consent and record the exact device settings used for each session so patient charts stay clear and defensible.
Cost Analysis & Purchasing Strategies for Shockwave Therapy Machines

Shopping for a shockwave therapy machine? Prices run wide, so it helps to think in three simple tiers: entry-level radial units near $10,000, mid-range hybrid models, and premium focused machines that often top $30,000. Refurbished units typically shave off about 20 to 30 percent. And leasing or installment plans can keep your upfront cost much lower.
Here are the common buying routes and what to expect:
- New purchase (full warranty, latest tech).
- Refurbished devices (lower cost, usually a shorter warranty).
- Lease or lease-to-own (smaller initial payment, regular monthly fees).
- Financing (spread payments over months or years).
- Extended warranty (adds coverage beyond the usual 1 to 3 years).
- Service contract (regular maintenance and faster repairs).
Think about return on investment as patient volume and price per session. Let’s keep it simple: charge $150 per session and plan for an average of 3 sessions per patient. That equals $450 in revenue per patient.
Quick math: $450 per patient means a $30,000 focused machine needs roughly 67 patients to pay for itself ($30,000 ÷ $450 ≈ 67). A $12,000 radial unit needs about 27 patients. That could look like six patients a month to break even in a little over a year for the focused unit. Wait, let me clarify that, your monthly pace changes how fast you recover the cost.
| Machine | Price | Break-even Patients (@ $150 x 3) | Months at 6 Patients/Month |
|---|---|---|---|
| Focused | $30,000 | ~67 | ~11 |
| Radial | $12,000 | ~27 | ~5 |
| Refurbished example (20% off focused) | $24,000 | ~54 | ~9 |
Leasing or financing eases cash flow, but it usually pushes break-even further out because you’re paying interest or monthly fees. Refurbished units lower the break-even count, but consider adding a service plan since warranties can be shorter.
Practical tips: project your expected annual treatments, factor in downtime for repairs, and compare warranty terms. Oh, and here’s a neat trick, run two scenarios: conservative and optimistic patient volume. Then see how each affects time-to-break-even. It makes the choice feel more like planning and less like a gamble.
In truth, pick the path that fits your clinic’s cash flow, expected patient load, and comfort with service risk. You’ll sleep better knowing the numbers line up with your day-to-day.
Top Shockwave Device Brands & Practitioner Testimonials
Three makers show up most often in clinic rooms: Storz Medical, Zimmer MedizinSysteme, and BTL Industries. They all offer radial and focused platforms (focused targets deeper tissue; radial spreads across a wider area), plus a variety of handpieces and preset programs that busy therapists rely on. Clinics usually choose a brand by matching signature models to their case mix, some like compact, portable units; others want full-featured consoles with preset libraries.
Have you noticed the same trend? Survey results are encouraging. About 88% of chronic-pain patients report improvement after shockwave treatment, and many providers see more than 95% device uptime. Practitioners often mention clean, easy-to-read interfaces, steady energy delivery, and vendor reps who jump in quickly when help is needed, so scheduled care keeps moving.
- Ease of operation – intuitive touchscreens and preset programs let staff set up quickly and treat more patients per day.
- Effective pain relief – clinics report fast symptom drops, especially for plantar fasciitis and chronic tendinopathies. Think of it like a focused nudge that helps tissue reset.
- Minimal downtime – rugged builds and high reported uptime mean fewer interrupted clinic days. Relax. Your schedule stays steadier.
- Strong technical support – manufacturers commonly offer training, quick repairs, and phone or on-site help so clinicians feel confident with settings and safety. Oh, and many include starter protocols that save weeks of trial and error.
Shockwave Therapy Devices Improve Rehab Outcomes
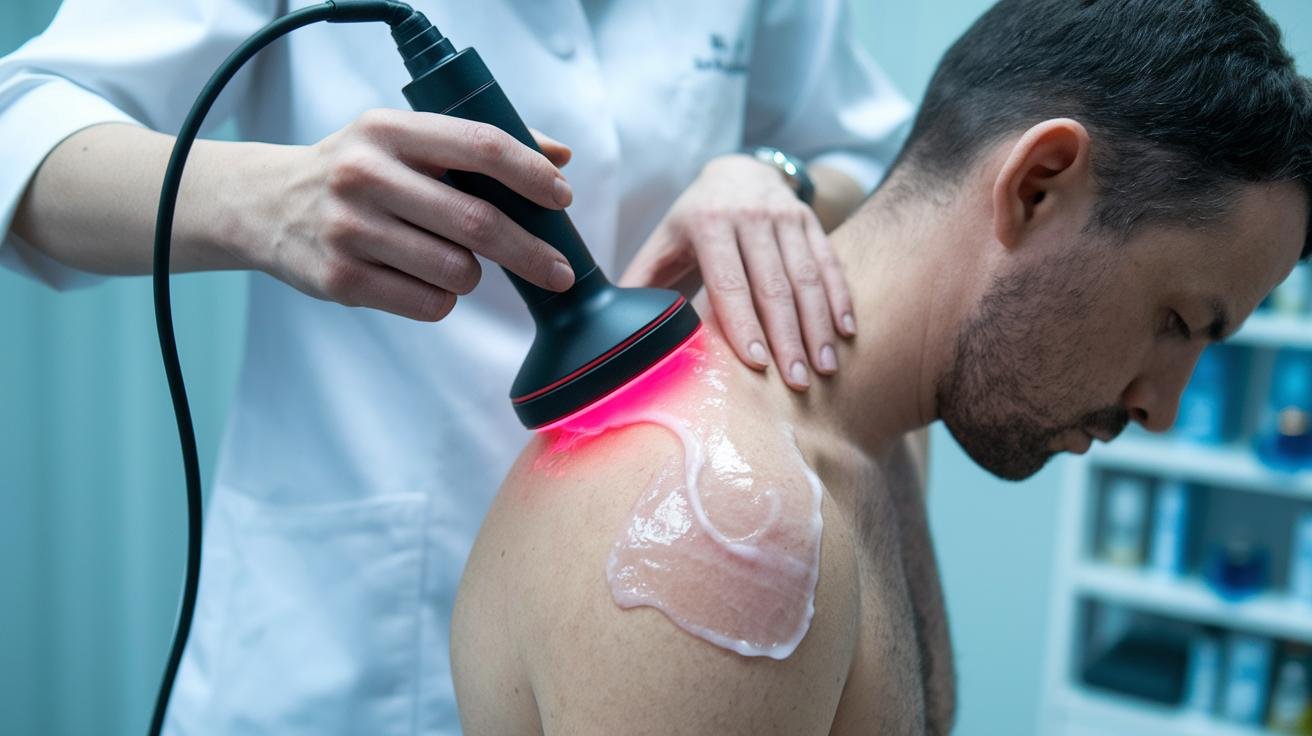
Before ESWT (extracorporeal shockwave therapy), start with a focused pre-treatment assessment. Take a clear history, examine the painful spot, and check neurologic and vascular status. If the diagnosis or lesion depth is unclear, review imaging. Get informed consent and record baseline pain and function scores so you can track changes.
- Position the patient so the target area is exposed and supported, letting the muscles relax. Small adjustments make a big difference for comfort.
- Apply a generous layer of ultrasound coupling gel and press out air pockets so the waves travel steadily through the skin. Think of it as making a smooth path for the pulses.
- Choose energy and frequency based on tissue depth and patient tolerance. Focused devices report energy as mJ/mm² (energy density); start low and titrate. Radial devices use bar pressure (a measure of air-driven force); set frequency in the 1-21 Hz range. Typical programs are 3-4 sessions, once a week.
- Pick the applicator head size to match the area , smaller tips (10 or 15 mm) for trigger points, larger tips (20 or 35 mm) for broader muscle surfaces. Match the tool to the tissue.
- Set pulse count and intensity. Most protocols deliver about 2,000-4,000 pulses per session, with treatment times around 5-15 minutes. Adjust intensity for patient comfort , slow increases work well.
- Run safety checks: confirm there are no contraindications, verify good coupling, check machine calibration and handpiece condition, and have emergency contact details handy. Safety first.
- Document everything: device settings, pulse count, applicator used, and the patient’s feedback in the chart. You’ll thank yourself at follow-up.
Aftercare matters. Ask patients to rest the treated area for about 24 hours and to avoid NSAIDs for roughly 48 hours so the body’s natural inflammatory steps can occur. Return to activity slowly. Ice briefly for acute soreness, and skip deep tissue massage for 48-72 hours. Reassess pain and function before the next session. Expect gradual gains across the 3-4 weekly sessions; if progress stalls, tweak parameters and reassess.
Emerging Innovations & Future Trends in Shockwave Therapy Devices

Broad-focused systems like SoftWaveTRT combine radial and focused wave generation with electrohydraulic reflectors (metal surfaces that redirect shockwaves to shape the energy field). That mix creates a more even energy field that reaches both surface tissue and deeper layers. Many patients describe it as a steady, warming sweep across the treated area, and folks tend to prefer that feel.
Modern units pair that hardware with smart software , real-time feedback, built-in treatment libraries, and over-the-air updates , so clinics can keep protocols current and track outcomes without extra fuss. Think of it like a smart assistant for treatment: it helps you stay consistent and learn what works over time.
Researchers are also exploring low-energy shockwave approaches for aesthetic and regenerative uses, like scar softening, skin remodeling, and wound-support therapies. The idea is gentle nudges to cells , fewer sessions, less discomfort, and targeted signals that encourage repair without heavy force. Early clinical reports and pilot studies are showing encouraging signs for faster recovery and better patient comfort. Oh, and some of the early results feel promising enough to keep watching closely.
Future focus areas include:
- Integrated EHR connectivity, for seamless documentation and protocol syncing with patient records.
- Wireless power solutions, so devices are truly cordless and easier to take on outreach visits.
- AI-driven parameter optimization, offering smart suggestions for energy, frequency, and pulse counts based on outcomes data.
Have you tried a newer unit yet? It’s like bringing a gentler, smarter hand to care.
Final Words
We jumped right into how shockwave tech moved from kidney-stone care to musculoskeletal therapy, then split into radial (broad, superficial) and focused (deeper, higher energy) options. We walked through clinical success rates, device specs, safety and maintenance, cost choices, leading brands, treatment protocols, and fresh innovations.
Think about the conditions you treat and the clinic setup, small choices add up to smoother sessions and happier patients. Choosing the right system can bring calm, targeted relief and better sleep, and shockwave therapy devices are a practical tool for that.
FAQ
Frequently Asked Questions
What is the best shockwave therapy device?
The best shockwave therapy device matches your condition and setting: focused FSWT for deep, chronic tendinopathies and calcifications, radial RSWT for superficial, broad muscle or tendon pain, plus the right energy and applicator sizes.
Can I do shockwave therapy at home?
You can do some low-energy radial shockwave therapy at home with consumer units, but depth and power are limited; talk with a clinician, follow instructions, and use proper coupling gel for safe treatment.
Can anyone buy a shockwave therapy machine?
Anyone can buy certain machines, but many models are marketed to licensed clinics; local rules and FDA/CE clearances vary, so check regulations, required training, and warranty before purchasing, including refurbished options.
Does shockwave therapy work for shoulder pain?
Shockwave therapy helps calcific shoulder tendinopathy, with focused FSWT showing about 70–80% success in studies; improvements often appear after several sessions and side effects are usually mild and short lived.
What about shockwave therapy devices for ED?
Shockwave therapy devices exist for erectile dysfunction (low-intensity ESWT); evidence is mixed and some uses are still investigational—discuss options with a urologist and confirm device clearance locally before treatment.
How do radial and focused shockwave devices differ?
Radial devices deliver lower-energy waves over wider areas for superficial issues; focused devices send higher-energy waves deeper for chronic tendinopathies and calcifications, chosen by target depth, energy units, and applicator size.
What should clinicians look for in a professional shockwave machine?
Clinicians should look for adjustable energy/frequency, multiple applicator sizes, built-in protocols, reliable warranty and maintenance plans, plus portability and strong manufacturer support to match practice needs.